
While in Custody: The Fight to Stop Jail Deaths in Washington State
STEPHANIE DEAL WANTED her mom to bail her out. She wanted to go home. To see her daughter, Ella. “It’s only, like, $40,” she pleaded over the phone from the Cowlitz County Jail.
The 29-year-old had been arrested in Longview, Washington, 100 miles south of Seattle, Saturday, August 3, 2013, on a charge of driving with a suspended license. But her mother, Jule Crowell, was hopeful. Finally, Crowell thought, Stephanie had hit rock bottom. Maybe she’d give up heroin. There was cash saved up for rehab when she was released. Ella, age six, could continue to live with Crowell and her husband for now. Things would get better.
And so, certain her tough love was the wisest choice, Jule Crowell told her daughter no. She would not bail her out.
The decision would haunt Crowell for years.
Early in the morning, a week after Stephanie’s arrest, the phone rang again. Crowell rose from her bed and hurried to the kitchen. She needed to go to the hospital, the voice mail message said—now. Her husband stayed behind with Ella, and Crowell drove the 10 miles to the emergency room. There, a hospital employee pulled her aside.
Crowell absorbed the information in a daze. Her daughter was dead. How could this have happened?, she thought. I just talked to Stephanie three days ago. She was in a safe place.
Months later, in November, the county gave Crowell the autopsy report. It only raised more questions. The manner of death was undetermined. The cause was unexplained.

Stephanie Deal died in the custody of the Cowlitz County jail in August 2013.
Stephanie Deal was among 16 people who died in custody in Washington state in 2013, and one of 967 people who died in custody in the United States that year. That’s according to the U.S. Bureau of Justice Statistics, the only agency to collect in-custody death data from jails across the country. Since it took on the task in 2000, the bureau has tallied nearly 15,000 jail deaths nationally. About half of those deaths were the result of an illness such as heart disease, while nearly a third of the detainees who died killed themselves. About 7 percent—or 1,017 inmates—died from drug or alcohol intoxication. The rest were counted under one of four other categories: accident, homicide, missing information, and other or unknown.
In 2014, the most recent year the bureau has official data for, 19 of the 1,053 people who died in jails perished in Washington state. Jails in Washington aren’t required to report in-custody deaths to any state agency, however, and federal reporting is voluntary. So the number could, in fact, be greater.
State representative Roger Goodman believes the disclosure of jail deaths is haphazard and inconsistent. “We just happen to hear about it,” he said. The state law requires that, at a minimum, jails meet “federal and state constitutional requirements relating to health, safety, and welfare of inmates and staff,” but there are no other regulations or enforcement.
Goodman is the chair of the House Public Safety Committee and a sponsor of a bill during the last session that would have established a joint legislative task force on jail standards. The bill left Goodman’s committee but was never voted on by the house.
While there is consensus among lawmakers, civil rights organizations, and law enforcement—there are too many residents with mental illness behind bars, jails are overwhelmed and underfunded—not everyone agrees that mandatory oversight is the solution to inconsistent care across the state. The Washington Association of Sheriffs and Police Chiefs, or WASPC, favors voluntary accreditation standards that the organization devised in 2014. Ned Newlin, WASPC’s jail services liaison, says that diverting more low-level offenders into community resources—rather than placing them in jail—would help reduce the chance of an in-custody death. But, he said, there’s no silver bullet. Each case is unique and needs to be evaluated individually. “Our jails are really trying to do the best they can given the resources that they have,” he said.
Columbia Legal Services recently filed requests with each jail in the state for all publicly available information about deaths that have occurred there in the past 10 years. But broad exemptions to the state’s public records laws shield many jail records from scrutiny, said Nick Straley, an attorney with the advocacy organization. Some jails have redacted nearly everything in response to the requests, including the inmate’s name. That makes it hard to figure out if an inmate’s death was preventable, Straley said, and to what extent poor medical care was responsible.
Jule Crowell is certain Cowlitz County could have prevented her daughter’s death and, in February 2014, she sued the county in federal court. Stephanie, who lost 17 percent of her body weight during the week she was jailed, “died a terrible and easily preventable death,” the lawsuit says. The county, it claims, killed her.
When Stephanie Deal was a girl, her mother would stick a Bette Midler cassette in the car stereo, open the sunroof, and drive her daughter and a friend to Portland, an hour south, to go shopping. On one trip, when they were stopped at a red light, Deal hit a high note and the pedestrians on the sidewalk burst into applause. She sang in her school chorus. She took dance lessons until she was 12. Crowell and her husband—Stephanie’s stepfather—dutifully attended her recitals.
She could be a drama queen. “If she cut her finger,” Crowell recalls, “you’d think she cut her finger off.”
She earned a certified nursing assistant license after high school and cared for the elderly in town. She became pregnant with Ella and continued working after she was born, taking time to bring her daughter to doctor appointments and speech therapy. Ella wasn’t speaking when other children her age started babbling, but it wasn’t until she was two that she was diagnosed with autism. Jaxen, a son, was a born a year later.
Crowell doesn’t know when Deal started using heroin. When she lost weight, Stephanie claimed she was on diet pills. She finally admitted she had a problem in the summer of 2012, when she and the kids moved into the guesthouse on her mother’s property. Crowell started paying for her to visit a methadone clinic in Vancouver, Washington.
But a year later, in June 2013, Crowell kicked her out. Stephanie was using again, and Jaxen’s father, who Crowell disapproved of, had been sneaking into the guesthouse. Ella stayed with the Crowells, and Jaxen moved in with his dad’s parents. Crowell urged Stephanie to get the help she needed. Then, on August 3, she was arrested.

Jule Crowell is suing Cowlitz County for the death of her daughter, Stephanie Deal.
She had been stopped at an intersection when a Longview police officer drove through it and noticed she wasn’t wearing a seat belt. When he ran her license number he learned she had a suspended license. She was booked at the Cowlitz County Jail. It wasn’t until the next day that she informed corrections officers she was withdrawing from heroin.
Another certified nursing assistant from Portland, booked in the same cell as Deal, noticed something amiss before that. Deal was vomiting so frequently that the woman grew alarmed and repeatedly tried to summon medical help, she later said in a declaration filed in court. She told jailers that Deal was becoming dehydrated. The officers told the nursing assistant to stop and cursed at and threatened her, the declaration states. “To see an obviously very sick person ignored,” she said, “was and continues to be a frightening episode for me.”
Three days later, a family friend who once worked with Stephanie was booked in the same unit. It was covered in vomit, she said in a declaration, and she saw Stephanie fall five or six times as she tried to make it from her bunk to the toilet. Once, walking to call her mom, she fell and hit her head and appeared unconscious, the friend said. Someone took her blood pressure and officers brought her back to the cell where she continued to vomit. When the friend called for help, people she believes were nurses told Stephanie to “stop faking” and “get up,” according to the declaration.
The lawsuit alleges blood work done by jail staff confirmed Stephanie was in serious medical trouble, and yet no care or treatment was provided until early August 10, when she had deteriorated to the point where she was incoherent and couldn’t respond. They waited too long to call an ambulance, the suit says, and Deal was pronounced dead at the hospital.
Captain Chris Moses at Cowlitz County Corrections declined to comment on the case due to pending litigation. In a response to the lawsuit filed in federal court in 2014, however, the county “denies liability and maintains that reasonable medical treatment was provided to Stephanie Deal while she was incarcerated.”
Conmed, which provides health care services for the jail and is also a defendant in the lawsuit, claims that Stephanie was seen multiple times by medical nurses and doctors and received prescriptions for medication, including for vomiting and diarrhea. A doctor ordered the jail to follow detox protocol, and Stephanie was twice moved from her cell to the medical unit as needed, according to court documents Conmed filed in the case. The health care provider claims dehydration couldn’t have killed Deal, as the lawsuit alleges. And it appears to blame her deteriorating health that morning on the medics who took her to the hospital. She threw up and choked on her vomit after they placed her on a gurney, according to the documents. (The company that employs the medics declined to comment on the allegations because of health care privacy concerns and the lawsuit.)
Nathan Roberts, one of Crowell’s attorneys, says the county and Conmed (now known as Correct Care Solutions) customarily deny meaningful medical care to detoxing inmates. Another Cowlitz County inmate, Jenny Borelis, was booked in the jail on May 12, 2013, and died of cardiovascular collapse after she was found on her cell floor on May 15, according to documents Roberts filed in court. Another, Daniel Bush, was booked at the jail on January 13, 2014, and died of pneumonia on January 20. Cameron Kuanoni was booked on January 29, 2014, and hanged himself with a bedsheet four days later. Like Deal, all three were detoxing. Their parents are also now suing the county.
When Jule Crowell and I met with one of her lawyers, Duane Crandall, in January, he gave me a photocopy of a recent newspaper article about the death of another woman at the jail. Britney Helene Smith, a 26-year-old arrested on a drug-related charge, was found dead in her cell on December 29, 2016. The cause was still under investigation in January, according to The Daily News. The paper noted that Smith was the sixth person to die at the jail since 2013.
“Our department takes it very seriously,” the paper quotes Corrections Department director Marin Fox Hight as saying. “We express our condolences to her friends and family.”
On October 9, 2015, a corrections officer noticed an emergency call light in the Pierce County jail cell of Matthew Smith. Smith told the officers that the pain in his abdomen was so severe he could barely walk or stand. A nurse transferred him to the jail’s medical clinic. This wasn’t the first time Smith had complained of health problems. Since his arrest in late August, the 48-year-old, who lived with Crohn’s disease and bipolar disorder, had regularly requested mental health care and alerted nurses to cramping, chest pains, and loose stools. On one occasion, toward the end of September, more than 20 reported episodes of diarrhea coupled with dehydration, nausea, and shortness of breath sent him to Tacoma General Hospital. The hospital’s discharge instructions advised the county that Smith should see a gastroenterologist or return to the ER if the symptoms became worse.
After officers delivered him to the jail’s clinic in a wheelchair on October 9, according to a lawsuit his family filed, he waited unattended. Seven hours later they found him lying on the floor by the toilet, bleeding from his rectum. He was pronounced dead 40 minutes later.
The cause of death was sepsis due to an inflamed j-pouch, a cavity formed from the small intestine to replace the colon, according to a postmortem examination report. Crohn’s disease is also listed as a significant condition. The suit brought by Smith’s parents, Ben and Nona, holds Pierce County and NaphCare, which provides medical care in the jail, responsible. Matthew would still be alive, the suit maintains, if officers and nurses hadn’t neglected his health while he was in custody.
Ben and Nona were visiting family in Alaska when Smith was arrested by Bonney Lake police on August 27, 2015, on charges of assault, reckless driving, criminal trespass, and obstructing an officer. At booking a nurse interviewed him and noted he would likely experience methamphetamine withdrawal. He admitted to using the drug three to four times a week and asked to be seen by a mental health professional. He claimed a man had been talking to him in his Bluetooth before his arrest, directing him to take off all his clothes and to drive as fast as he could to somewhere safe.
Ben Smith had seen his son break from reality before. He thinks Matthew was “living in another world” before he was arrested. “I’ve done some things that are probably going to alter my life,” he told his dad on the phone from jail one day. Together they worried about car insurance. How would he be able to afford it after a reckless driving arrest? But the next time they spoke, Ben was more concerned about his son’s health. He could hear it in his voice. After nearly five decades, he knew what sick sounded like.

Nona and Ben Smith say they’re reluctantly suing Pierce County in order to obtain an explanation of why their son Matthew (featured on the opposite page) died in jail.
The second of three boys Ben and Nona Smith raised in Bonney Lake, Matthew was a quiet kid who drummed in the high school band and once marched more than five miles in the Rose Parade. He was a Boy Scout. He played the Tin Man in The Wizard of Oz in the third grade. Once he caught a trout at Lake Ethel and kept it in a coffee can in his dresser, until his mom discovered it a week later. When he was about 14, doctors discovered ulcers in Matthew’s stomach and, roughly two years later, diagnosed him with Crohn’s, an inflammatory bowel disease.
He grew up in the house Ben Smith built his family back when the family could afford to buy a lot but not a home. Now the walls are covered in quilts Nona has stitched and photos of their boys captured in time, fishing, backpacking in the Olympics, going to prom. In most of the shots Matthew looks boyish with light blond hair and a slight smile. Nona says he grew a beard to look older.
He never grumbled when his parents took him to the doctor or if he was in pain. But in that jail he did.
After his son’s death, Ben Smith turned the dining room into an office, spreading the autopsy report on the table. He wanted answers. He says he called the sheriff’s office several times but could rarely get someone to speak to him. When he did, he says, they wouldn’t say much. In July 2016, the couple filed a lawsuit.
Pierce County did not respond to my multiple requests to discuss the case either. Bradley Cain, general counsel for the jail’s health provider, called Smith’s death a tragedy but declined to comment further: “NaphCare intends to respect the integrity of the litigation process and will address and defend against those allegations,” he said.
Ben Smith is suing Pierce County, reluctantly, he says, because he feels he has no choice. “They won’t even talk to me.” The 73-year-old shrugged and slapped the table gently. His face trembled. “I’m not sure I’ll live long enough to see this thing through.”
Nona peered across the table at Erik Heipt, an attorney who accompanied me to their house in November. A plate of peanut butter cookies she had made was resting on the table. She stared down at the lace tablecloth for much of our meeting. As I asked about her son, she wiped away tears from behind her glasses. Ben steadied his own scratchy voice and recalled memories of Matthew’s youth and of the day they found out he had died—the worst day of their lives. Now Nona had a question. She wanted to know how other counties respond when someone dies in their custody. “Do they usually answer the questions?”
The Smiths’ lawyers, Edwin Budge and Erik Heipt, met at law school, at Willamette University, in Salem, Oregon, and upon graduation in 1994 they formed Budge and Heipt, a civil rights firm in Seattle. The pair focused on employment cases, suing companies on behalf of people who believed they were wrongfully fired, until the early aughts, when they took on their first jail death.
Sandra Morgan, in Texas, had called dozens of lawyers looking for someone to accept her case. Her son Kevin Bledsoe had died in Jefferson County, 50 miles northwest of Seattle, on the Olympic Peninsula, in 2001. She was looking for justice.
Bledsoe, a single father who’d recently moved to Washington from San Antonio, had been partying at a trailer in Port Hadlock on March 24, 2001, when he “flipped out,” friends told The Port Townsend and Jefferson County Leader. He ran to a nearby QFC and broke a window on a parked pickup truck. Somebody called the cops. A scuffle ensued, but officers were able to subdue Bledsoe with pepper spray, a hood over his head, and hog-tying restraints.
At around 1:10am, the officers brought Bledsoe to the Jefferson County jail’s crisis cell, a bare concrete room for detainees who pose a danger to themselves or others. They placed him on his stomach on a mattress on the floor and held him down while he was stripped and his restraints were replaced with leg irons. When they left, the deputies thought they could hear snoring.
Minutes later, corrections officer Hank Shafer checked in on him. Bledsoe’s lips and ears were turning blue. Medics drove him to the hospital in Port Townsend. At 2:51am a doctor pronounced him dead. A medical examiner determined he had died from methamphetamine toxicity.
Sandra buried her son in a family plot in Bluffton, Texas. Then she started researching his death. She pored over newspaper stories and the autopsy report. She wrote down what she considered hints and contradictions in a notebook that grew to be three inches thick. When she hired Heipt and Budge in 2003, they retained Dr. Richard Cummins, a professor of medicine at the University of Washington, to review the case. Cummins concluded that Bledsoe’s death was “imminently preventable.” Asphyxiation due to ventilation restriction killed him, he said; not meth.
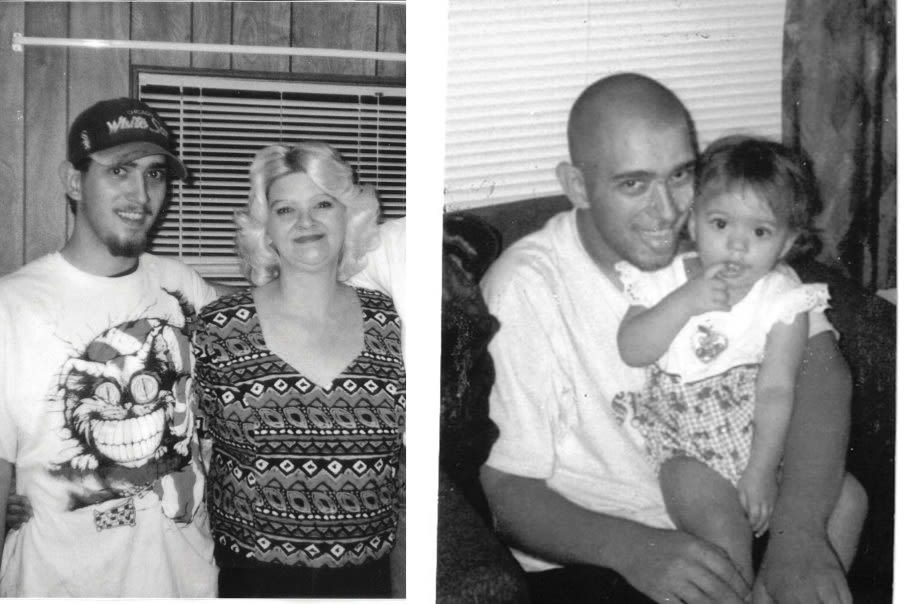
Kevin Bledsoe with his then-two-year-old daughter, Kaitlyn (right). He was pronounced dead two years later, in Port Townsend. Kevin (left) with his mother, Sandra Morgan.
Image: Courtesy Sandra Morgan
Steve Richmond, the jail superintendent for Jefferson County, agrees that the death was avoidable. But he blames Bledsoe. “He could’ve prevented it, absolutely—by not taking methamphetamine,” Richmond said. “His heart exploded due to the meth ingestion.”
Richmond defends the officers’ actions. “These guys faced a combative, out-of-control individual. They prevented further injury to themselves and others by the actions they took to restrain him and get him into custody. Once in custody, the restraints were removed as soon as allowable.”
None of the arresting officers involved were disciplined. Two are now captains at the sheriff’s office, and another is a sergeant. The only corrections officer on duty at the jail that night, then a recent graduate from the training academy, is now a U.S. marshal.
For corrections officers, fielding a steady stream of criminal suspects with a variety of behavioral and physical health needs can be daunting. Franklin County sheriff Jim Raymond said it’s hard for law enforcement to assess the health needs of inmates suffering from mental illness or addiction. They should be getting the help they need outside of jail, he said. “Society just wants to point the finger at the local sheriff.”
Ned Newlin, the jail services liaison for WASPC, said the criminal justice system has become a de facto mental health provider since the mental health system was deinstitutionalized in the 1980s. But as jails have been expected to provide care for more people, there has not been more funding, Newlin said. “Why are these people even coming into the jail? What are the failings of our social network? What’s happening in the community?”
Budge and Heipt spent more than a year readying for trial, collecting depositions from the deputies and statements from law enforcement and medical professionals. In October 2004, the county settled for $1.6 million.
In a photo posted on Facebook a decade after his death, Kevin Bledsoe appears with his daughter, Kaitlyn, then two years old. She’s wearing a blue-and-white checked dress covered in cherries, her finger hooked in her mouth. Her eyes are big and hazel, like her dad’s. She was almost four years old when he died.
“I had to grow up real fast,” Kaitlyn, now 19 said in December. She was sitting in the San Antonio house she bought with money she received in a separate settlement with the county for $130,000, bouncing one of her own sons on her knee, four-month-old Thanos. As a kid, when friends would ask where her father was, she’d respond coolly that he had been murdered in Washington. It wasn’t until she talked to Heipt and Budge in Seattle in late 2015 that she learned of her father’s final hours.
“The uncovered civil rights issue of our time, in my opinion, is preventable deaths in county jails,” says Heipt, “of people who have not been convicted—not even sentenced.” Though they’re not dying from a gunshot wound or a blow to the head, Heipt says, there’s nothing natural about inmates who suffer a fatal withdrawal, seizure, or heart attack if they’re deprived of medication, medical attention, or a drug they’re dependent on.
Back in Longview, Jule Crowell is still coming to terms with the realization that her grandchildren will grow up without a mother. Even as Stephanie Deal struggled with addiction, Crowell says, her children were her cornerstone. She cooked and cleaned and took them to the park, and when she lived away from them, she visited.
Ella is now in fourth grade and Jaxen is in kindergarten. In the fall, he and his classmates drew on whiteboards. Jaxen drew his mom on the ground and himself standing over her, crying. The arrow pointing up meant she was going to heaven, he said. Crowell and the kids release balloons to the sky on Stephanie’s birthday and eat her favorite dessert, shortbread layered in cream cheese, pudding, Cool Whip, and nuts. Crowell made it for her every year. Now they’re making Stephanie a memorial garden. “I think the kids need it just as much as I do,” she said.
Crowell is still reckoning with her decision to not rescue her daughter when she pleaded for bail. She knew Stephanie was an addict and needed help; she didn’t know she was so sick. “I would’ve got her out,” she says, tears streaming down her cheeks. “I have to live with that for the rest of my life.”
And she worries about something else. She worries that the cops and the jails—the whole system, really—don’t treat addicts the way they treat other citizens, that they consider her daughter and others like her nobodies.
“Well they were once a somebody,” she says. “And they still are.”




