
A Navy Vet's Indefinite Recovery from Long Covid
Photo: Teresa and Dennis Sionson.
Dennis Sionson was lacing up his Adidas one April morning when his world dimmed. The 57-year-old Navy man had battled sickness for several days, his exhaustion so severe that he finally green-lit a trip to the doctor with his wife, Teresa. Probably just a bad cold, he’d thought. But as the couple prepared to leave for the Naval Health Clinic near their Oak Harbor home, Dennis’s breaths grew shorter, his face paler. His vision faded and, in an instant, went completely dark, like someone had switched off the light. His wife watched him crumple to the floor.
The ambulance came quickly after Teresa’s 911 call, whisking Dennis away to WhidbeyHealth Medical Center. His plummeting oxygen level demanded a ventilator. For days the machine sustained him as he fought a raging case of Covid-19, the disease caused by the new coronavirus that had already hospitalized more than 2,000 Washingtonians by the time he arrived at the Coupeville facility on April 2.
Five days after his admittance, Dennis was helicoptered to University of Washington Medical Center in Seattle for more care. Some in the ICU feared that Dennis, tethered to a ventilator for weeks, wouldn’t make it. But over the next three and a half months, the hospital’s treatments would save Dennis, who ultimately suffered a stroke, lung injury, polyneuropathy, and brain damage.
Since the pandemic’s outset, few post-Covid patients have spent this much time rehabilitating the very basics of their being: walking, swallowing, breathing. Dennis wouldn’t leave the hospital until July 21.
Two months before that, he awoke to cheers. He’d finally tested negative for coronavirus. Staffers rejoiced. Dennis, meanwhile, couldn’t yet breathe on his own, let alone celebrate. Or speak.

The soul moves first, Alissa Smith would stress to Dennis. The body would need more time. Smith started her speech-language pathology sessions with him in late May, when he was still bedridden in the ICU and weeks away from walking. His care team had removed his ventilator and inserted a tracheostomy tube, giving him an extra passageway to breathe. The tubing’s positioning ensured that he couldn’t “make a voice yet,” Smith recalls. Face scrunches and scribbled notes (when he wasn’t too tired) would have to suffice for communication. But Dennis also had to conquer something even more fundamental than speaking: He had to learn how to swallow again.
On their first day together, Dennis gulped barium so that Smith could assess his swallowing performance by x-ray. Disturbingly, she found liquids and solids moved into his airway and toward his lungs instead of his stomach.
Tubes fed Dennis for months. Even as he learned to keep food down, his memory posed an obstacle to retention. His illness had damaged the “white matter” connections in his brain, impairing his cognition and coordination. “I know that it’s kind of hard to remember some things now,” Smith would tell him, “and I don’t really know how much easier that’s going to get.”
Dennis belongs to a growing community of survivors who still endure the virus’s torment long after two-week quarantines and hospital stays. While scientists trained much of their attention early in the pandemic on the disease’s polar effects—lethal and asymptomatic—researchers are increasingly studying its lingering toll on those who have never fully recovered. In perhaps the most extreme finding, roughly 87 percent of a previously hospitalized Italian cohort experienced at least one symptom two months, on average, after the disease’s onset.
Some patients, dubbed “long-haulers,” report symptoms of extreme fatigue, brain fogginess, and chills months after their positive test. And Covid-19 patients are particularly susceptible to post-intensive care syndrome, an umbrella term for persistent physical, cognitive, and psychological complications born from prolonged ICU stays. “My concern is that a lot of these patients will not necessarily bounce back, and that you get this infection in your 30s and your entire life is now changed,” says Dr. Aaron E. Bunnell of UW Medicine’s Department of Rehabilitation Medicine.
Inpatient clinics at Harborview Medical Center and UW Medical Center have marshaled expertise in treating critical illnesses and brain injuries to help post-Covid patients achieve some degree of recovery. Many exercises focus on retraining lungs compromised by acute respiratory distress syndrome (ARDS)—a hallmark of Covid-19 that profoundly affects survivors’ endurance, according to Bunnell. Telehealth appointments often keep those breathing regimens on track.
But a video consult couldn’t simulate the lunches Dennis shared with Alissa Smith after he shed his ventilator and learned to swallow again. Dennis kept requesting more information, rehearsing his swallows, stomaching barium tests. Gradually, Smith’s exercises drew him closer to normal modes of consumption as he moved from the hospital’s ICU in Seattle’s Montlake neighborhood to an acute care floor and, ultimately, to the rehab unit. A bite of yogurt was a revelation.
Over that period, his voice returned, first meekly through a speaking valve attached to his tracheostomy tube, later resoundingly as he sang the hymns he’d recite back home. A week and a half before his discharge from the hospital, he could restart a full diet. Smith wasn’t surprised. “There was no way he wasn’t going to be eating and drinking by the time he left.”

Stoic. Resilient. Badass. That’s how members of Dennis’s care team at UW describe Dennis as he persevered in the ICU and rehab. “He’s one of the hardest workers I’ve ever met in my life,” says occupational therapist Henry Giang. “I don’t know if anyone else could survive what he went through.”
Giang and others credit the patient’s military background. Born in Manila, Dennis joined the U.S. Navy as part of a long-running recruitment program that permitted Filipinos to enlist without first immigrating to the country, a dream for Dennis. In 1988 he reported to Oak Harbor, where Naval Air Station Whidbey Island stands 90 miles north of Seattle, and never left. Over a three-decade career, he ascended the ranks to maintenance master chief petty officer, tending to aircrafts and overseeing well over 100 people before his retirement in 2017. He hadn’t been counting the days. Chopping it up with the sailors was too fun. “Time passes by really quick,” he says.
Coronavirus can rearrange that temporal flow, he’d learn when he first experienced its wrath. As his condition worsened at home, Dennis hallucinated. He responded to Teresa with “yessir,” promised to report to the “FRC”—the Fleet Readiness Center where he’d stopped working years earlier. “Like he was in the Navy,” Teresa says.
Before Dennis fell ill, Teresa had experienced the virus’s scourge at a remove, learning about its symptoms on TV. Now, it was in her own home, in her husband. “It’s like you’re watching a movie,” she says, “and you’re a part of the movie now.”
Except Teresa couldn’t actually witness the scenes unfolding inside the ICU at WhidbeyHealth and, later, UW Medical Center. Hospital guest restrictions during the pandemic prevented her from seeing Dennis until May 29. After nearly two months of FaceTiming doctors, she could finally visit her husband. As soon as Teresa was allowed in, Alissa Smith recalls, she would almost never leave his bedside, diligently taking notes.
Teresa had prayed for her husband. This absence was far more fraught than any of his Navy deployments. “There’s a date when you’re coming back,” Dennis says of those stints away from Teresa and their sons, Matthew and Marvyn. “But when I went through Covid, she didn’t know when I’m coming back, or if I’m coming back.”
In late June, nearly three months after he collapsed over his shoes at home, Dennis doubles over in a shower at UW’s Montlake rehab center, straining to breathe. Occupational therapist Henry Giang has wheeled him to the walk-in, stationed about 15 feet from the room where Dennis now sleeps. Giang had thought his new patient was ready for his first proper shower since entering the hospital. In bed, his oxygen saturation rate had sat at 96 percent, comfortably above the unofficial 90 percent threshold for normal breathing. But when Dennis bends over to wash his thighs on this day, crunching his lungs, the number dives to a perilous 78 in a matter of seconds. “It was one of the scariest moments of my life,” recalls Giang, who would summon a nurse to help quell Dennis’s racing heart.
The 31-year-old therapist had seen only a handful of people as sick as Dennis when the two met on June 24. Many of his coughing fits lasted upwards of a minute. In healthy patients, lungs appear clear in x-rays. Dennis’s were veiled in white. “It was like looking through a trash bag,” Giang says.
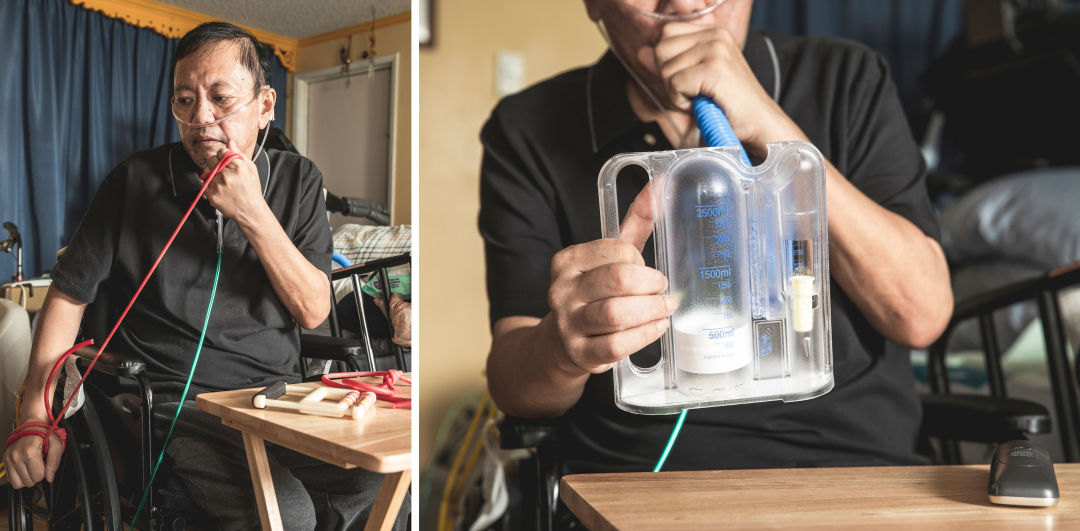
Still on oxygen, Dennis strains to rebuild his basic strength and lung capacity.
His sessions aimed to boost Dennis’s memory, strength, breathing, and endurance to levels that would support the kinds of daily functions a healthy person takes for granted: bathing, dressing, grooming, toileting. Between these activities, the two would often repeat respiration exercises common to many recoveries.
Still, it was uncharted territory for Giang. He’d only seen one other coronavirus patient at that point in the pandemic, and reliable research about the new disease was scant. He devised a four-week therapy program based in part on his knowledge of strokes and ARDS, the lung leakage that had wreaked havoc on Dennis’s breathing. He also learned as he went. He noticed, for instance, that tight muscles contributed to shorter inhalations and limited expansion of his chest cavity. To loosen him up, he applied cupping and other massage techniques, which appeared to spur deeper breaths and higher oxygen levels.
The occupational therapist pushed his patient—“whatever was medically possible, without killing him,” says Giang. On days when Dennis looked like he’d gone on “a 50-mile hike,” Giang would concentrate on, among other things, rebuilding the patient’s finger muscles, letting him rest. But most of the time, Dennis was game to be stretched to the limit. He bonded with his OT over a shared affinity for food, including lumpia and other Filipino fare. He even ribbed Giang when the therapist dressed him after the shower incident. “You panicked, man,” Dennis teased.
While Giang pushed Dennis to the brink to restore his daily life functions, physical therapist Laura Wessbecher gradually trained him to walk beyond his immediate surrounds. The ovular rehab unit served as their makeshift track, Dennis counting tiles on the floor as, bit by bit, they rounded a 200-foot loop.
Initially, he could move only 30 to 50 feet with a four-wheeled walker before needing to sit down. Polyneuropathy had led to persistent numbness and weakness in his left leg. A brace on his left ankle propped up his weakened foot as they ambled down hallways. The drag on his gait didn’t prevent him from graduating to a cane instead of a walker for short distances, and his range on wheels extended to 150 feet. Progress, but a long way from the two-mile runs he used to take pre-coronavirus, when the vet didn’t have to field orders on how to brush his teeth and comb his hair. Was he ever frustrated? No, he says. “I’ve been working on my second life.”
Dennis’s current reality revolves around a hospital bed that occupies a sizable chunk of his living room in Oak Harbor. As he recounts his ordeal shortly after his release, his voice is a wheeze between coughs. An oxygen tube bisects a sunken face. His sturdy 194-pound frame has withered to 152. An oxygen machine now anchors a man who was once always on the go and never sick to his living room.
A nurse checks in with him at home, where Teresa tends to him assiduously. Telehealth appointments track and guide his ongoing rehab. Dennis’s first video call evoked sessions with Giang—exhale for four seconds, inhale for two. The occupational therapist gave Dennis a bunch of tools to cope with the next stage of his recovery. A reacher akin to a trash picker to grab his laundry off the floor. A sponge to scrub his back. A sock aid and shoehorn because, for all his gains, Dennis can’t tie his shoes yet without assistance. “I’m still far away from my old self,” he says.
Physically, cognitively, but not spiritually. Dennis doesn’t lament what he’s lost. “I’m at peace,” he says. He’s grateful for the care of his medical team, for the prayers of his wife and friends. Because even as coronavirus seized his body, his soul never left.




